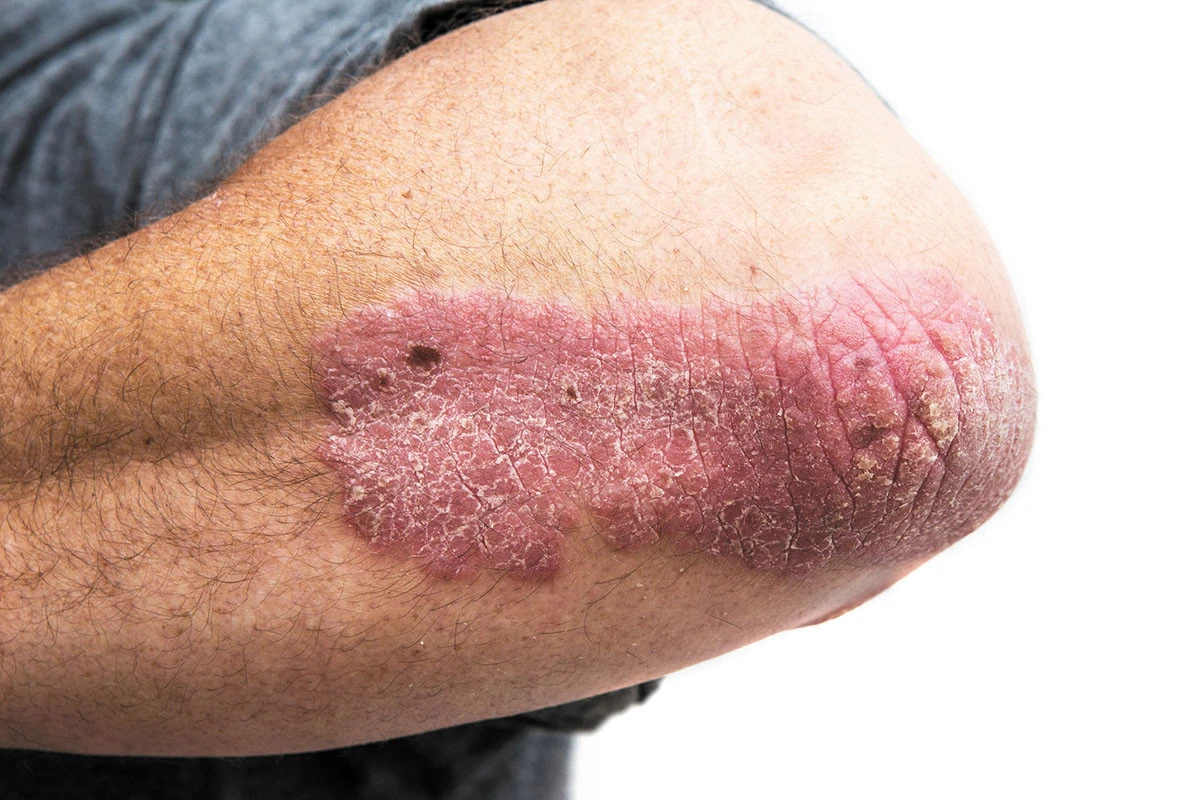
Psoriasis is a chronic inflammatory skin condition that affects millions of people worldwide, causing discomfort, embarrassment, and often profound emotional distress. Characterized by red, scaly plaques on the skin, psoriasis can impact not only physical health but also mental well-being and quality of life. Despite its prevalence and long history, psoriasis remains a complex and enigmatic condition, with much still to be learned about its underlying causes and optimal management. In this overview, we delve into 25 intriguing facts about psoriasis, shedding light on its genetic predisposition, diverse manifestations, historical significance, treatment milestones, and future directions in research and care. By understanding the multifaceted nature of psoriasis, we can better support those living with this challenging condition and work towards improved outcomes and quality of life.
Family Affair (1): Psoriasis has a strong genetic link, as indicated by the American Academy of Dermatology. If one parent has psoriasis, there’s a 10% chance that a child will develop it. This risk increases to 25% if both parents are affected. The genetic predisposition to psoriasis involves multiple genes, and inheriting certain combinations of these genes can increase susceptibility. However, while genetics play a significant role, environmental factors also contribute to the development and severity of psoriasis. Understanding the genetic component of psoriasis is crucial for both diagnosis and developing personalized treatment approaches.
Skin Cell Sprint (3-4 days): In healthy skin, cells typically take about a month to mature and shed. However, in psoriasis, this natural cycle accelerates dramatically to just 3-4 days. This rapid turnover of skin cells leads to the accumulation of immature cells on the skin’s surface, resulting in the characteristic thick, scaly plaques associated with psoriasis. The exact mechanisms driving this accelerated cell turnover are complex and involve dysregulation of the immune system, as well as abnormalities in signaling pathways within the skin. Understanding the underlying biology of this process is essential for developing targeted therapies that can normalize skin cell proliferation and differentiation.
Koebner’s Phenomenon (up to a third): Koebner’s phenomenon refers to the development of new psoriatic lesions at sites of skin trauma or injury. Up to a third of people with psoriasis experience this phenomenon, which can occur in response to various forms of skin trauma, including cuts, scrapes, burns, or even insect bites. The exact mechanisms underlying Koebner’s phenomenon are not fully understood but may involve a localized inflammatory response triggered by injury, which then promotes the development of psoriatic lesions in genetically susceptible individuals. Recognizing and minimizing skin trauma is important for managing psoriasis and preventing the exacerbation of symptoms.
Not Just Skin Deep (40%): Psoriasis is not just a skin condition; it can also affect the joints, leading to a condition known as psoriatic arthritis. Up to 40% of individuals with psoriasis develop psoriatic arthritis, which is characterized by joint pain, swelling, stiffness, and progressive damage. Psoriatic arthritis can significantly impair mobility and quality of life if left untreated. The exact relationship between psoriasis and psoriatic arthritis is complex and involves both genetic and environmental factors. Early diagnosis and aggressive management are crucial for preventing joint damage and preserving function in individuals with psoriatic arthritis.
Celebrities with Psoriasis: Psoriasis can affect anyone, including celebrities like Kim Kardashian and Jon Hamm, who have openly discussed their experiences with the condition. By sharing their stories, these individuals have helped raise awareness and reduce the stigma surrounding psoriasis. Their openness about living with psoriasis has also inspired others to seek treatment and support. Psoriasis does not discriminate based on fame or fortune, and knowing that even well-known figures struggle with the condition can be empowering for those facing similar challenges.
Ancient Awareness (300 BC): Psoriasis is not a modern ailment; medical descriptions of the condition date back to ancient times. The Greek physician Hippocrates, often regarded as the father of Western medicine, referenced psoriasis as “psora” in his writings dating back to around 300 BC. Despite its long history, psoriasis remains a complex and enigmatic condition, with much still to be learned about its underlying causes and optimal management strategies. The recognition of psoriasis throughout history underscores the enduring impact of this chronic inflammatory disorder on human health and well-being.
Flakes by the Pound (1 pound per week): The extent of skin shedding in psoriasis can be astonishing, with individuals experiencing moderate to severe forms of the condition shedding up to 1 pound (0.45 kg) of skin cells per week. This excessive shedding contributes to the visible scaling and flaking characteristic of psoriatic plaques. The sheer volume of shed skin cells underscores the intense metabolic activity and dysregulation occurring within the skin of individuals with psoriasis. Effective management of psoriasis involves not only reducing inflammation and promoting skin healing but also addressing the underlying factors driving this abnormal skin turnover.
Sunlight Savior (80%): While excessive sun exposure can exacerbate certain skin conditions, moderate sunlight exposure can actually benefit some individuals with psoriasis. Up to 80% of people with psoriasis experience improvement in their symptoms with moderate sun exposure. Sunlight helps suppress inflammation in the skin and promotes the production of vitamin D, which has immune-modulating effects. However, it’s essential for individuals with psoriasis to balance sun exposure with sun protection measures to prevent sunburn and skin damage. Consulting with a dermatologist can help determine the appropriate amount of sunlight exposure for individuals with psoriasis.
Stress Response: Stress is known to play a role in exacerbating psoriasis symptoms in some individuals. The exact mechanisms underlying the link between stress and psoriasis are not fully understood but likely involve complex interactions between the nervous system, immune system, and endocrine system. Stress can trigger inflammatory responses in the body, which may exacerbate existing inflammation in the skin and worsen psoriasis symptoms. Managing stress through relaxation techniques, mindfulness practices, and lifestyle modifications may help reduce the frequency and severity of psoriasis flare-ups in susceptible individuals.
Mediterranean Marvel: Emerging research suggests that adherence to the Mediterranean diet, which is rich in fruits, vegetables, whole grains, legumes, nuts, seeds, and healthy fats like olive oil, may help improve psoriasis symptoms. The Mediterranean diet is renowned for its anti-inflammatory properties, thanks to its abundance of antioxidants, omega-3 fatty acids, and polyphenols. These nutrients can help modulate the immune system and reduce systemic inflammation, which are key factors in the pathogenesis of psoriasis. While dietary modifications alone may not be sufficient to manage psoriasis, adopting a Mediterranean-style eating pattern as part of a comprehensive treatment plan may complement other therapies and improve overall health outcomes.
Famous Fingernails: Psoriasis can affect the nails, causing characteristic changes such as pitting, discoloration, and separation from the nail bed. These nail changes, known as nail psoriasis, can be distressing and may also lead to functional impairment. Nail psoriasis is often challenging to treat and may require specialized interventions, such as topical or intralesional medications, to improve nail health and appearance.
Oil Change: Individuals with psoriasis often have lower levels of vitamin D, a vital nutrient that plays a role in immune regulation and skin health. Supplementation with vitamin D may be recommended by healthcare professionals to help optimize vitamin D levels and potentially improve psoriasis symptoms. However, the use of vitamin D supplementation in psoriasis management should be carefully monitored and tailored to individual needs, as excessive vitamin D intake can have adverse effects.
Teenage Trouble: While psoriasis can affect individuals of any age, onset often occurs during adolescence or early adulthood, typically between the ages of 15 and 25. The hormonal changes associated with puberty, as well as genetic and environmental factors, may contribute to the development of psoriasis during this period. Psoriasis onset during adolescence can significantly impact self-esteem and social functioning, highlighting the importance of early diagnosis and intervention to minimize the psychosocial burden of the condition.
Global Reach: Psoriasis is a prevalent condition, affecting an estimated 125 million people worldwide. This widespread prevalence underscores the global impact of psoriasis on public health and healthcare systems. Despite its high prevalence, psoriasis remains underdiagnosed and undertreated in many parts of the world, leading to significant disparities in access to care and quality of life for affected individuals.
Invisible Impact: Beyond its physical symptoms, psoriasis can have a profound impact on mental health, leading to increased rates of anxiety, depression, and diminished quality of life. The visible nature of psoriatic plaques can contribute to feelings of self-consciousness, social isolation, and low self-esteem, further exacerbating psychological distress. Recognizing and addressing the psychological impact of psoriasis is essential for providing comprehensive care and improving overall well-being in affected individuals.
Treatment Timeline: The history of psoriasis treatment dates back to the 19th century when coal tar was first documented for use as a topical treatment. Coal tar preparations have been used for their anti-inflammatory and antipruritic properties in managing psoriasis symptoms. Since then, significant advancements have been made in psoriasis treatment, including the development of topical corticosteroids, phototherapy, systemic medications, and biologic therapies, offering a range of options for patients based on the severity and characteristics of their condition.
Breakthrough Biologics: The late 20th century saw a revolutionary development in psoriasis treatment with the introduction of biologic drugs. Biologics target specific components of the immune system involved in the pathogenesis of psoriasis, such as tumor necrosis factor-alpha (TNF-alpha), interleukin-17 (IL-17), and interleukin-23 (IL-23), thereby providing targeted and effective treatment options for moderate to severe psoriasis. Biologic therapies have transformed the management of psoriasis, offering improved efficacy, safety, and quality of life for many patients who were previously refractory to conventional therapies.
Psoriasis Awareness Month: Every July, organizations worldwide observe Psoriasis Awareness Month to raise awareness about the condition, advocate for improved treatment options, and support individuals living with psoriasis. Psoriasis Awareness Month provides an opportunity to educate the public, healthcare professionals, policymakers, and affected individuals about the impact of psoriasis on physical and mental health, as well as the importance of early diagnosis, access to care, and research advancements in psoriasis management.
Scalp Sensitivity: Psoriasis commonly affects the scalp, resulting in symptoms such as itching, flaking, and the formation of thick, crusted patches. Scalp psoriasis can be particularly challenging to manage due to the presence of hair, which can interfere with topical treatments and make application difficult. Specialized shampoos, corticosteroid solutions, tar-based preparations, and phototherapy may be used to effectively treat scalp psoriasis and alleviate associated symptoms.
Guttate Psoriasis: Guttate psoriasis is a less common subtype of psoriasis characterized by the sudden onset of small, red, teardrop-shaped lesions scattered across the skin. This type of psoriasis is often triggered by a bacterial or viral infection, such as streptococcal throat infection, and typically affects children and young adults. Guttate psoriasis may resolve on its own or progress to chronic plaque psoriasis, requiring appropriate management and follow-up care to prevent complications and recurrence.
Emotional Rollercoaster: Psoriasis is characterized by a cycle of flare-ups and remissions, leading to significant emotional turmoil for affected individuals. The unpredictable nature of the condition, combined with its visible symptoms and impact on daily functioning, can contribute to feelings of frustration, anxiety, and depression. Managing the emotional aspects of psoriasis is essential for holistic care and may involve psychotherapy, support groups, and coping strategies to help individuals navigate the challenges of living with a chronic skin condition.
Hungarian Waters: Bathing in mineral-rich water from the Dead Sea, located between Israel and Jordan, has been used for centuries as a therapeutic approach to managing psoriasis symptoms. The unique composition of Dead Sea water, which is rich in minerals such as magnesium, calcium, and potassium, is believed to possess anti-inflammatory and skin-soothing properties. Dead Sea baths, along with other complementary therapies such as phototherapy and topical treatments, may help alleviate psoriasis symptoms and improve overall skin health.
Gut Feeling: Emerging research suggests a potential link between gut health and psoriasis, highlighting the role of the gut microbiome in modulating immune function and inflammation. Imbalances in the gut microbiome, known as dysbiosis, have been observed in individuals with psoriasis, suggesting a possible connection between gut health and disease pathogenesis. Strategies aimed at promoting gut health, such as dietary modifications, probiotic supplementation, and lifestyle interventions, may complement existing psoriasis treatments and improve clinical outcomes.
Tech Revolution: The advent of telemedicine has transformed the landscape of psoriasis care, making it easier for individuals to access consultations, support, and follow-up care from healthcare professionals remotely. Telemedicine platforms allow patients to connect with dermatologists and other specialists through virtual appointments, video consultations, and secure messaging systems, overcoming barriers such as geographic distance, transportation issues, and scheduling constraints. Telemedicine has the potential to enhance access to care, improve patient satisfaction, and optimize treatment outcomes for individuals with psoriasis.
Future Hope: Researchers are continually exploring new treatment options for psoriasis, including innovative approaches such as gene therapies aimed at achieving long-term remission and disease modification. Gene therapies target specific genetic and molecular pathways implicated in psoriasis pathogenesis, offering the potential for more precise and personalized treatment strategies. While gene therapy for psoriasis is still in the early stages of development, ongoing research holds promise for groundbreaking advancements in the field of psoriasis treatment, with the ultimate goal of improving outcomes and quality of life for affected individuals.
Here are 5 FAQs about Pshoriasis:
- What is psoriasis and what causes it?
Psoriasis is a chronic autoimmune disease that affects the skin. In healthy skin, cells grow and shed in a predictable cycle. But in psoriasis, this process goes into overdrive. The immune system sends mistaken signals, causing skin cells to multiply too quickly. This rapid turnover creates thick, red, scaly patches on the skin.
The exact cause of psoriasis remains unknown, but it’s believed to be a combination of genetics and environmental triggers. If you have a close family member with psoriasis, you’re more likely to develop it yourself. Certain triggers, like stress, infections, medications, and even injuries, can also bring on a flare-up.
- Is psoriasis contagious?
Absolutely not! Psoriasis is an autoimmune condition, not a contagious disease. You cannot catch it from someone else through physical contact or by sharing personal items. The underlying cause lies within the body’s immune system, not any kind of transmissible virus or bacteria.
- Are there different types of psoriasis?
Yes, psoriasis manifests in several forms, each with slightly different characteristics. Here are some of the most common types:
Plaque psoriasis: This is the most common type, affecting around 80% of people with psoriasis. It causes raised, red plaques with silvery white scales, typically on the elbows, knees, scalp, and lower back.
Guttate psoriasis: Often triggered by a strep throat infection, this type appears as small, red, teardrop-shaped lesions, mainly on the torso and limbs. It’s most common in children and young adults.
Inverse psoriasis: This form affects smooth areas of the body like the armpits, groin, and genitals. The patches are typically red, inflamed, and less scaly compared to plaque psoriasis.
Pustular psoriasis: This less common type is characterized by white pustules (tiny pus-filled bumps) on red, inflamed skin. It can appear in localized areas or cover the entire body.
Erythrodermic psoriasis: This rare and severe form involves widespread redness, scaling, and intense itching across most of the body’s surface. It requires immediate medical attention.
- Is there a cure for psoriasis?
Unfortunately, there is no permanent cure for psoriasis. However, there are many effective treatments available to manage symptoms and improve quality of life. These treatments can include:
Topical medications: Creams, ointments, and lotions containing steroids, corticosteroids, or vitamin D can help reduce inflammation and scaling.
Phototherapy: Controlled exposure to ultraviolet (UV) light can slow skin cell growth and improve psoriasis symptoms.
Medications: Oral or injected medications like methotrexate and cyclosporine suppress the overactive immune system response.
Biologic drugs: These newer, targeted drugs work by specifically inhibiting specific proteins involved in the inflammatory process of psoriasis.
- How can I manage psoriasis and live well with the condition?
While there’s no cure, there are many ways to manage psoriasis and maintain a good quality of life. Here are some tips:
Work with your doctor: Develop a personalized treatment plan and discuss any concerns you have.
Identify your triggers: Stress, infections, and certain medications can worsen psoriasis. Try to identify and avoid your triggers whenever possible.
Maintain a healthy lifestyle: Eat a balanced diet, exercise regularly, and get enough sleep. These habits can contribute to overall well-being and potentially improve psoriasis symptoms.
Manage stress: Techniques like yoga, meditation, and deep breathing can help manage stress, which can trigger flare-ups.
Join a support group: Connecting with others who understand the challenges of psoriasis can be a source of encouragement and valuable information.